|
In many of the cases, there were aspects of treatment that were potentially negligent however, this aspect of management is not the subject of this review and did not affect the data collected.ĬES is a constellation of clinical symptoms and signs, not all of which have to be present to make a diagnosis of CES, and many are not present when CES is diagnosed. In 11 of these cases, surgery was performed within 24 hours of the MRI scan, and in two, there was a delay (2 days and 3 days) despite the diagnosis being clear retrospectively. voluntary voiding was possible and took place before the PVR was measured. All cases were classified as CESI, as there was executive control of bladder emptying, i.e. In all cases, the MRI scan was done within 24 hours of the PVR assessment. In all 13 cases, the cause of cauda equina compression was a lower lumbar disc herniation, eight being at the L4/5 level and five at the L5/S1 level. In one case, there was doubt about the diagnosis, and we therefore excluded it from analysis, leaving 13 cases where there was a clinical diagnosis of CES, confirmed by MRI, and where emergency surgery was performed. In 14 of these, the PVR volume was 200 ml or lower. Of 50 medicolegal cauda equina syndrome cases, 26 had records of PVR being measured. These are summarised in the diagram (Fig. for a positive MRI scan, namely “a large lumbosacral disc prolapse occupying most of the canal cross-sectional area sufficient to compress the CE… ”.Īll cases have been anonymised and have no identifying data in accordance with the World Medical Association Declaration of Helsinki statement of ethical principles for medical research. We used the same criteria as Katzouraki et al. In cases where the PVR was ≤ 200 ml, we recorded the following: age, sex, bladder symptoms, urinary and/or bowel incontinence at any time, subjective and clinician-tested impairment of perineal sensation, reduced anal tone, level of compression on MRI, confirmation of diagnosis by a radiologist and surgeon, the clinical decision to perform emergency decompression, and the timing of surgery. We identified those cases where the PVR was recorded. 
The reports were prepared for both claimants and defendants. We retrospectively reviewed the two senior authors’ 50 most recent medicolegal reports that concerned patients who were litigating in relation to CES. Whilst we value the assessment of objective measures to diagnose cauda equina syndrome and support the widespread use of bladder scanning, we wish to document our experience that cauda equina syndrome requiring emergency decompression can still be present when a PVR is less than 200 ml. in 1992 went even further and stated that “the predictive value of a negative test (no urinary retention) would be almost 0.9999”. have stated that if the PVR is ≤ 200 ml, and there are no clinical signs of CES, the probability of a negative MRI is 98.7%, and such patients do not require emergency MR imaging. 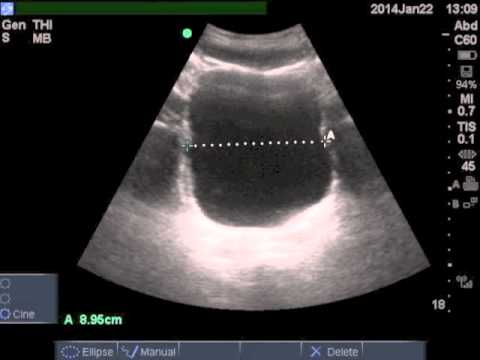
The residual volume of urine present in the bladder post-void (PVR) has been proposed as an accurate assessment of the probability of a patient having CES. Bladder ultrasound is a cheap, noninvasive assessment of bladder function, which is widely available in emergency departments. 
This leads to high rates of negative MRIs in patients who have suspected CES. Many symptoms and signs are quoted as “red flags” for CES but none reliably predict cauda equina (CE) compression on MR imaging. There is no universally agreed definition of CES. The failure to diagnose and treat CES before there is permanent and/or severe neurological injury is important for all patients and is also important medicolegally. Early diagnosis and treatment of CES can prevent harm. The CES is a condition that can lead to severe disabling symptoms causing long-term social and medical morbidity.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
